Pediatric Patients
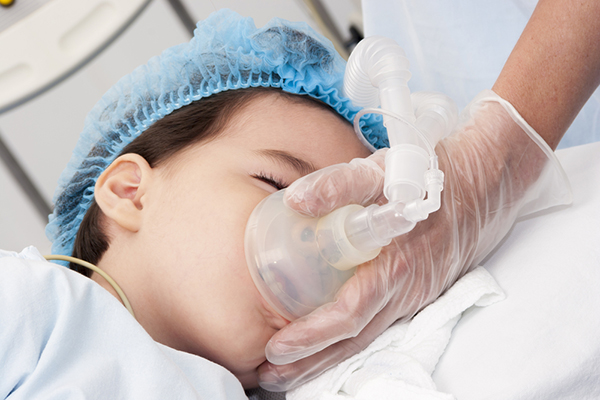
Anesthesia/Sedation can be safely administered to children in a suitably equipped dental office and many procedures for children are often done in such a setting. Children benefit from the early return to comfortable and familiar surroundings. Parents benefit because of less time away from other family members and less interruption in their work schedules. In most cases, your child will be familiar with the surroundings where the procedure will be performed since it will be done in their dentist’s office.
Most children do quite well during their dental treatment; however children who are apprehensive or undergo extensive dental rehabilitation often require sedation to have their dental needs met.
Sedation is a state of sleep, which not only allows your child to be anxiety and pain free during his/her dental treatment, but also allows the dentist to deliver his or her best dentistry for your child.
Consulting with your child’s pediatrician and your child’s pediatric dentist will determine if your child is a candidate for in-office sedation.
Frequently Asked Questions
What about eating or drinking before my child's anesthesia?
– Your child should not eat any solid food for at least 6 hours before the arrival time.
– Your child may have up to 8 ounces of clear liquids up to 2 hours prior to the arrival time.
– Your child may have breast milk up to 4 hours prior to the arrival time.
– Your child may have up to 6 ounces of infant formula or milk up to 6 hours prior to the arrival time.
Note: Examples of clear liquids are water, apple juice, clear tea and Jell-O (not red)
Should my child take his/her usual medicines?
It is important to discuss this with your anesthesiologist. Continue to give your child his/her medications unless your anesthesiologist instructs otherwise.
What should my child wear?
– Please dress your child in a loose-fitting, short-sleeved t-shirt.
– Please remove all your child’s jewelry.
What should I bring to the appointment?
– Please bring a laundered blanket to keep your child warm during the procedure.
– Please bring a change of clothing for your child.
What happens before the procedure?
Your anesthesiologist will contact you a day or two before your appointment to obtain your child’s current medical history and to discuss any co-existing medical conditions your child may have. Pre-Sedation/Anesthesia instructions as well as all your questions and concerns will be discussed at this time.
What happens on the day of the procedure?
– Parents should plan to stay in the office during your child’s procedure and to make every attempt to have siblings stay at home.
– Upon arrival at the dental office, the anesthesiologist will conduct a pre-operative interview and physical examination and discuss the anesthetic plan with you.
– If your child is healthy, you and your child will be escorted to the operatory at which point an IV will be started followed immediately by a small amount of sedative. EKG, BP Cuff and Pulse Oximetry for vital monitoring and interpretation are then applied. At this point, you will be asked to sit in the reception area until the procedure is completed and your child is awake.
What happens during the procedure?
– For most children, deep sedation is the preferred form of anesthesia.
– Your anesthesiologist is responsible for managing your child’s care and will be with your child throughout the procedure. He/She will monitor your child’s vital signs and ensure your child’s safety.
– During the surgery, your child will rest comfortably and will have no recollection of the procedure.
– At the end of the procedure, your anesthesiologist will slowly wake your child up and he/she will be transferred to you in a private room for full recovery. Your anesthesiologist will discuss post-operative instructions with you at that time. It usually takes 30 to 60 minutes before your child will be fully discharged to your care.
Will my child have any side effects?
– Your anesthesiologist will administer pain medication prior to your child waking up to reduce the effects of post-operative pain.
– Although nausea or vomiting is rare after these procedures, the occurrence may be related to anesthesia and the ingestion of blood tinged saliva. Your child will be given medication to control and suppress post-operative nausea and vomiting.
– A dry, scratchy throat and a dry, bloody nose are also common due to the oxygen administered during the procedure.
– Your child may experience a low grade fever several hours after the procedure. This is a normal reaction to the events of the day and is not necessarily a sign of infection.
When will we be able to go home?
After a thorough and comprehensive post-operative evaluation, if your child meets the criteria for discharge, your anesthesiologist will discharge and send your child home with post-anesthetic instructions. Most patients are ready to go home between 30 minutes and 60 minutes after the surgery is completed.
What instructions will I receive?
– Both written and verbal instructions will be provided after your child’s procedure.
– All questions will be answered and you should feel comfortable taking your child home.
What can I expect during my child's recovery at home?
– Most children often take a two hour nap after their procedure and will want something to eat and drink when they wake up. Please refrain from giving them something to eat or drink until after two hours after their procedure is over.
– Some children may also experience a sore throat and occasional dizziness or headaches. Nausea may be present, but vomiting is less common.
– These side effects usually decline rapidly in the hours following your child’s procedure.